Automating Community Pharmacy Workflows: The Impact of RPA on Operational Efficiency and Patient Care
Wirun Wetsiri1,* and Worapat Paireekreng2,*
1College of Innovative Technology and Engineering, Dhurakij Pundit University, Bangkok, Thailand
2King Mongkut’s Institute of Technology Ladkrabang, Bangkok, Thailand
E-mail: 65140011@dpu.ac.th; worapat.pa@kmitl.ac.th
*Corresponding Authors
Received 18 October 2024; Accepted 19 March 2025
Abstract
This study investigates the impact of Robotic Process Automation (RPA) on operational efficiency, error reduction, and patient care within community pharmacies. Adopting a mixed-methods approach, we evaluated four key pharmacy workflows – automated prescription dispensation, inventory management, patient follow-up, and medication ordering – across 12 pharmacies. Quantitative data were collected through structured questionnaires (N 120) and performance measurements (e.g., processing times in minutes per transaction), while qualitative insights were gathered via semi-structured interviews and direct observations. The findings reveal that RPA implementation reduced prescription dispensation time by 67% (from 15 to 5 minutes), medication ordering time by 83% (from 60 to 10 minutes), and patient follow-up time by 80% (from 40 to 8 minutes), with a corresponding increase in patient engagement of 66.7%. Survey data indicate a positive outlook among pharmacy personnel – 78% believe RPA can enhance efficiency and 75% are ready to adopt it, provided that comprehensive training and support are available. Despite these promising outcomes, challenges such as system integration complexity and financial constraints were identified. Based on these results, a structured RPA implementation framework is proposed, emphasizing comprehensive training, phased deployment, seamless integration, and active stakeholder engagement. Overall, this study underscores RPA’s potential to transform pharmacy operations, enabling a shift toward more patient-centered care while highlighting the need for strategic change management to ensure long-term success.
Keywords: Robotic process automation (RPA), community pharmacies, workflow optimization, prescription dispensation, inventory management, patient engagement, automation in healthcare, digital transformation, pharmacy operations, error reduction, healthcare technology, patient follow-up, medication ordering, operational efficiency.
1 Introduction
The emergence of Robotic Process Automation (RPA) has led to substantial progress across multiple sectors by automating repetitive and rule-based activities. In healthcare, especially inside community pharmacies, RPA offers a chance to augment operational efficiency, minimize errors, and elevate the quality of patient care. Pharmacies, as vital healthcare providers, encounter distinct obstacles in overseeing substantial administrative responsibilities, controlling inventory, filling prescriptions, and assuring efficient patient follow-up. These duties are frequently labor-intensive, susceptible to inaccuracies, and may divert attention from more value-enhancing activities like patient counseling and professional care. Consequently, the implementation of RPA in community pharmacy environments may enhance these workflows, enabling pharmacists to concentrate more on patient-centered care.
Recent studies indicate that RPA can markedly alleviate the load of repetitive administrative activities across diverse healthcare environments. It has been successfully implemented in hospital environments to automate patient registration, invoicing, and inventory management, leading to significant time savings and a decrease in errors. Nonetheless, studies regarding the implementation of RPA in community pharmacies are still scarce. This gap offers a chance to investigate the distinct advantages and obstacles of applying RPA in community pharmacies, especially in settings that differ markedly in operational scale, digital preparedness, and workflow intricacy.
This study aims to assess the efficacy of RPA in enhancing essential workflows in community pharmacies. The research concentrates on four prioritized pharmacy operations identified through initial interviews with pharmacy personnel: automated prescription dispensation documentation, inventory management automation, patient follow-up and notifications, and automated drug ordering. These activities were chosen due to their automation potential and their considerable capacity to enhance productivity and minimize errors.
A mixed-method research methodology was utilized to fulfill the study’s purpose, integrating qualitative and quantitative data collection techniques. The qualitative component comprised semi-structured interviews and direct observations to provide insights into existing process issues, perceptions of RPA, and preparedness for automation. The quantitative aspect encompassed the creation and implementation of RPA prototypes designed for specific pharmaceutical tasks, followed by an assessment of their effects on critical performance indicators, including processing duration, error frequency, patient interaction, and inventory management efficacy.
This study’s findings are anticipated to offer a thorough insight into the possible impact of RPA on community pharmacy workflows. This research seeks to illustrate the efficacy of RPA in diminishing manual workloads, reducing errors, and enhancing workflow efficiency, hence fostering the wider implementation of digital automation solutions within the pharmacy sector. Furthermore, it underscores the necessity of connecting technology advancements with the distinct requirements and contexts of community pharmacies, ensuring that these solutions not only improve operational efficiency but also assist pharmacists in providing superior patient care.
The next sections of this paper outline the literature review, research methodology, results, discussion, and conclusions, offering a comprehensive analysis of the influence of RPA on community pharmacy operations.
2 Literature Review
2.1 Adoption and Strategic Frameworks for RPA Implementation
The emergence of Robotic Process Automation (RPA) has transformed many sectors by automating repetitive, rule-based activities. In healthcare – especially within community pharmacies – RPA presents an opportunity to boost operational efficiency, reduce errors, and improve patient care quality. Community pharmacies often face unique challenges: managing high administrative workloads (e.g., prescription dispensation, inventory control, and patient follow-up) that are labor-intensive and error-prone. These challenges can detract from patient-centered tasks such as counseling and clinical care.
While RPA has been widely adopted in hospital environments to automate processes like patient registration, invoicing, and inventory management, thereby saving time and reducing errors, its application in community pharmacies remains less explored. This gap, characterized by differences in operational scale, digital preparedness, and workflow intricacy, calls for research that investigates both the advantages and obstacles of RPA in these settings. In this context, the current study focuses on four key pharmacy operations – automated prescription dispensation documentation, inventory management automation, patient follow-up and notifications, and automated drug ordering – selected for their high potential to enhance efficiency and reduce manual errors.
To achieve this, a mixed-method research design is employed: qualitative data are collected through semi-structured interviews and direct observations to understand existing process challenges and perceptions of RPA, while quantitative data stem from the development and implementation of RPA prototypes that are evaluated using performance indicators such as processing time, error rates, and patient engagement.
2.2 Robotic Process Mining (RPM): Optimizing RPA Utilization
Robotic Process Mining (RPM) is introduced as an adjunct methodology to improve RPA deployment by analyzing user interaction data (UI logs). Leno et al. (2020) [5] outline a seven-step process that includes UI log collection, noise filtration, segmentation, simplification, candidate routine identification, executable routine discovery, and final compilation. This systematic approach helps in identifying highly repetitive tasks that are ripe for automation.
Recent studies have furthered RPM’s application. Yadav and Panda (2022) [6] recommend integrating RPM with other methods – such as quantitative and survey-based approaches – to better identify suitable automation candidates. Moreover, Bahaweres et al. (2022) [7] have demonstrated that techniques like the Fuzzy Miner algorithm can refine repetitive operations and enhance overall efficiency in processes such as Purchase-to-Pay. Despite its promise, the practical use of RPM in community pharmacies is challenged by data privacy concerns; pharmacies handle sensitive patient and sales data, meaning that the use of UI logs must be carefully managed to avoid compromising data protection.
2.3 Checklist-Based Support for RPA Projects in Non-IT Environments
Given that many community pharmacy staff may not have extensive technical expertise, structured support is essential for successful RPA adoption. Wewerka and Reichert (2021) [8] propose a checklist-based framework to assist knowledge workers in managing RPA projects. This framework is divided into five phases:
• Evaluation: Determining which pharmacy processes are rule-based and repetitive, and estimating the potential resource savings.
• Preparation: Equipping staff with relevant information and training, and developing user-friendly RPA bots tailored to the specific needs of the pharmacy.
• Implementation: Deploying reliable and secure RPA solutions with thorough documentation and ongoing user feedback.
• Go Live: Ensuring a smooth transition through clear communication and comprehensive training.
• Maintenance: Continuously monitoring and updating RPA bots to adapt to changes in the pharmacy’s operations or IT infrastructure.
Building on this, Piyatilake et al. (2022) [9] emphasize that success in RPA projects is not solely dependent on technical skill but also on structured project management practices, including strategy alignment, effective user training, and clear communication. Additionally, Nielsen et al. (2023) [10] advocate for a benefits realization approach that considers cross-functional teams and top management support, ensuring that non-IT environments like community pharmacies can implement and sustain RPA initiatives successfully.
2.4 Implementing RPA in Healthcare: Insights from the NHS Framework
The NHS Transformation Directorate and Atos (2022) provide a comprehensive framework for designing, delivering, and sustaining RPA in healthcare settings. The report emphasizes that by 2022, 90% of large organizations globally will have adopted some form of RPA, with capabilities expected to triple by 2024. This framework, tailored to healthcare environments, can be adapted for use in community pharmacies to improve service delivery and efficiency [11].
The framework includes seven key components:
1. Understanding RPA: Evaluating the benefits, limitations, and case studies specific to the healthcare context.
2. Getting Started: Defining strategic goals for RPA, assessing organizational readiness, and selecting suitable technology solutions.
3. Demand Generation and Triage: Identifying and prioritizing processes that are ideal for automation based on their impact and feasibility.
4. Build and Develop: Using lean principles to design efficient and straightforward RPA workflows.
5. Release, Embed, and Run: Planning for RPA deployment, training staff, and providing support to ensure smooth operation.
6. Governance: Establishing policies, standards, and risk management frameworks to oversee RPA implementation.
7. Enablement: Providing continuous training, fostering collaboration, and encouraging innovation to sustain RPA initiatives.
Radke et al. (2020) [12] highlight that integrating RPA in healthcare – through automating tasks such as patient scheduling and claims processing – can lead to significant efficiency gains, which resonates with the framework’s objectives. Similarly, Sumathi and Jeyalakshmi (2022) [13] and Baumann and Cabassa (2020) [14] emphasize the critical roles of governance, data protection, and training in ensuring effective RPA adoption. Adapting these insights to the community pharmacy context helps ensure that automation aligns with both operational objectives and patient care standards.
2.5 Good Pharmacy Practice (GPP) Guidelines: Aligning RPA with Regulatory Standards
The Good Pharmacy Practice (GPP) guidelines, published by the Ministry of Public Health of Thailand (2014), outline the key roles and responsibilities of pharmacists in community pharmacies. These guidelines provide a foundational basis for identifying areas where RPA can be integrated to improve efficiency and maintain compliance with regulatory standards [15]. Recent studies support this alignment, demonstrating how GPP can serve as a framework for ensuring that RPA enhances both operational efficiency and compliance.
Key areas where RPA can be applied include:
• Medication and Inventory Management: Automating inventory tracking and medication dispensing to minimize errors and ensure the availability of essential drugs.
• Patient Interaction and Counselling: Using RPA to manage patient records and routine queries, freeing pharmacists to focus on more critical aspects of patient care.
• Regulatory Compliance: Ensuring that automated processes adhere to GPP guidelines, maintaining the quality of service and patient safety.
Bou-Saba et al. (2023) emphasize the significance of compliance with GPP criteria in community pharmacy, observing that numerous pharmacies do not achieve complete conformity, especially in dispensing, storage, and service quality. Their research highlights the necessity for enhancements in pharmacy procedures, proposing that technological innovations may facilitate improved compliance with GPP requirements by mitigating these operational difficulties [16].
Singu et al. (2023) document the results of facility inspections in Namibia, indicating that automation technologies such as RPA can aid in adhering to worldwide GPP standards. The research indicates that automated solutions may be especially advantageous in overseeing compliance-related activities, including drug storage, dispensing, and inventory management [17].
Punturungsee and Ploylearmsang (2023) illustrate the beneficial effects of technological solutions in assisting pharmacies to achieve GPP requirements in Thailand. Their research emphasizes that the implementation of RPA can optimize administrative functions and enhance adherence to GPP, resulting in increased operational efficiency and improved regulatory results [18].
Aligning RPA projects with GPP principles enables community pharmacies to improve operational efficiency while maintaining regulatory compliance. This guarantees that automated procedures comply with the utmost standards of service quality and patient safety.
2.6 Performance Analysis for RPA in Pharmacies
Quille et al. (2023) present a Performance Analysis Method for evaluating the impact of RPA in business processes, which can be adapted for community pharmacies. The framework consists of four key steps: understanding processes and architecture, identifying and selecting RPA processes, designing models based on system infrastructure, and analyzing and interpreting results [19]. This method enables pharmacies to:
• Select appropriate processes for RPA based on workload, process complexity, and financial benefits.
• Simulate and statistically analyze the performance of newly automated processes to optimize RPA usage.
• Develop strategies for effective RPA deployment, reducing risks associated with new technology investments.
Additionally, Khrystolubova et al. (2022) focus on defining appropriate quality performance metrics for pharmacies, specifically for those dispensing oral oncology therapies. Their study emphasizes the use of performance metrics in evaluating pharmacy services, which can serve as an important factor in assessing the overall efficiency and effectiveness of automated systems in pharmacy workflows [20].
Urick et al. (2021) discuss the design and effect of performance-based payment models in community pharmacies. The study highlights the role of performance measures and financial impact on pharmacy operations, which provides a useful perspective when considering the integration of automation technologies like RPA in community pharmacy settings [21].
By utilizing these performance analysis methods, community pharmacies can make more informed decisions about RPA implementation, ensuring that the technology delivers maximum value while aligning with both operational and financial objectives.
2.7 Technology Acceptance
To understand technology acceptance, several key theories on technology adoption and process optimization in healthcare are relevant:
• Technology Acceptance in Health Informatics: TAM and UTAUT
AlQudah et al. (2021) provide a systematic review of technology acceptance in healthcare, identifying TAM and UTAUT as the most prevalent models. Their study highlights that factors such as anxiety, computer self-efficacy, and trust significantly impact the acceptance of healthcare technologies across various settings. This influenced the inclusion of questions related to perceived usefulness, ease of use, and social influences in our questionnaire to gauge pharmacy staff’s readiness for RPA adoption [22].
• Diffusion of Innovations Theory
Dearing and Cox (2018) emphasized that innovation adoption in healthcare is affected by factors such as cost, complexity, and organizational readiness. This guided the development of questionnaire items addressing potential barriers to RPA adoption, helping to capture a comprehensive picture of the challenges within pharmacy operations [23].
• Acceptance and Use of Telemedicine Technology
Rouidi et al. (2022) focused on the acceptance and use of telemedicine among healthcare professionals, using the TAM and UTAUT models to understand the factors influencing adoption. Their work highlights the relevance of healthcare-specific considerations, such as trust and perceived usefulness, in the adoption of new technologies, which parallels our focus on RPA adoption in pharmacies [24].
• Impact of Trust and Privacy Concerns
Dhagarra et al. (2020) explore the impact of trust and privacy concerns on patients’ acceptance of technology in healthcare. Their findings underscore the importance of addressing privacy issues and building trust to encourage the adoption of new technologies like RPA in healthcare environments [25].
• Older Adults’ Intention to Use Medical Apps
Ma and Luo (2022) apply the UTAUT and TAM models to study older adults’ intention to use medical apps during the COVID-19 pandemic. Their results emphasize the role of perceived usefulness and facilitating conditions in shaping users’ willingness to adopt technology, which informed our approach to evaluating pharmacy staff’s readiness for RPA [26].
These frameworks informed the development of a questionnaire aimed at assessing key factors influencing RPA adoption in community pharmacies, providing a basis for effective implementation strategies.
3 Research Methodology
Objective of the Study
The objective of this study is to evaluate the effectiveness of Robotic Process Automation (RPA) in optimizing key workflows within community pharmacies. Specifically, the study examines whether RPA can automate repetitive and time-consuming tasks to enhance operational efficiency, reduce errors, and improve patient care. Four critical pharmacy activities – automated prescription dispensation recording, inventory management, patient follow-up/alerts, and automated medication ordering – were selected based on preliminary interviews with pharmacy personnel and stakeholder feedback.
Study Design
A mixed-methods approach was adopted to provide a comprehensive assessment of RPA’s impact on pharmacy workflows. This design combines qualitative data (from semi-structured interviews and direct observations) and quantitative data (from structured questionnaires and experimental performance measurements). The study design enables an in-depth understanding of both operational improvements and human factors affecting RPA adoption.
Questionnaire Development
To capture the perspectives of pharmacy personnel regarding RPA adoption, a structured questionnaire was developed. The questionnaire includes four sections:
1. General Information: Collects demographic data (e.g., age, gender, role) and professional background, including experience with digital technologies.
2. Opinions on Pharmacy Workflows: Explores perceptions of current workflow inefficiencies, repetitive tasks, delays, and error rates.
3. Attitudes Toward RPA: Assesses knowledge, past experience, perceived benefits, challenges, and overall acceptance of RPA technology.
4. RPA Implementation in Pharmacies: Investigates perceived challenges (financial, personnel, process, IT infrastructure), as well as support and training needs essential for successful RPA adoption.
The questionnaire was distributed to pharmacy staff across the selected sites. A total of approximately 120 respondents participated, ensuring a representative sample from both urban and rural settings.
Participant Selection and Setting
Twelve community pharmacies were purposively selected from diverse settings, including urban districts in Bangkok and rural areas. Selection criteria included:
• Geographical Diversity: Ensuring representation of both urban and rural contexts.
• Operational Engagement: Pharmacies actively involved in key activities targeted for automation (e.g., prescription dispensation, inventory management).
• Digital Maturity: A range of digital preparedness levels was considered to assess RPA’s adaptability across different operational scales.
Within these pharmacies, participants included pharmacy owners, pharmacists, managers, and support staff. This diverse group ensured insights from various perspectives regarding workflow challenges and technology adoption.
Qualitative Data Collection
Semi-Structured Interviews:
• Conducted with pharmacy owners, pharmacists, and staff (approximately 15 interviews).
• Focused on understanding current workflow challenges, attitudes toward RPA, and readiness for automation.
• Explored detailed expectations and concerns about automating tasks such as prescription dispensation and inventory management.
Direct Observations:
• Conducted in each of the 12 pharmacies to document existing workflows.
• Aimed to identify repetitive manual tasks and assess potential efficiency gains from RPA.
• Observations informed the design and refinement of the RPA prototypes
Quantitative Data Collection and Experimental Setup The quantitative component involved the development, deployment, and evaluation of RPA bots tailored to automate the prioritized pharmacy activities. Key aspects include:
• Automated Prescription Dispensation Recording:
An RPA bot was designed to extract prescription data from the pharmacy’s Point of Sale (POS) system and automatically populate forms on external state reimbursement platforms (e.g., KTB, Amed Care). Processing times were measured in minutes per transaction.
• Inventory Management Automation:
An RPA bot with Optical Character Recognition (OCR) capabilities was developed to automate data entry from delivery notes (Goods Received) into the POS system. This bot was tested for its ability to adapt to various document formats.
• Patient Follow-up and Alerts:
An RPA prototype was implemented to automate follow-up communications. It sends notifications (e.g., via LINE) and logs patient responses, thereby reducing follow-up time and increasing engagement. Pre- and post-intervention metrics (in minutes and percentage changes) were recorded.
• Automated Medication Ordering:
An RPA solution was developed to monitor real-time stock levels. When stocks reached a preset reorder point, the system generated purchase orders and emailed them to suppliers. The reduction in ordering time was quantified in minutes.
RPA Prototype Development: The prototypes were developed using no-code/low-code platforms such as Microsoft Power Automate and AppSheet. These platforms were chosen for their rapid deployment capabilities, ease of integration with existing systems, and cost-effectiveness for community pharmacies. Although these platforms offer flexibility, potential limitations (e.g., language compatibility or integration issues) were addressed through iterative testing and custom adaptations.
Data Analysis
Qualitative Analysis:
• Thematic analysis was conducted on interview transcripts and observation notes to identify recurring themes, challenges, and opportunities related to RPA adoption.
• Focus areas included perceptions of automation’s impact on workload, job satisfaction, and workflow efficiency.
Quantitative Analysis:
• Descriptive statistics were used to summarize questionnaire responses, including metrics such as average processing times, error rates, and engagement percentages.
• Inferential statistics, specifically paired sample t-tests, were applied to compare key performance indicators (e.g., processing time before and after RPA implementation). These tests justified the statistical significance of observed improvements.
• Data were collected over a defined period to ensure that “old time” and “new time” measurements were consistent and comparable (e.g., time per transaction measured in minutes).
Training and Support Considerations Given that successful RPA implementation depends on user readiness, a training program was developed to support staff throughout the study. The training addressed:
• Technical Training: How to interact with and troubleshoot the RPA tools.
• Operational Training: Process mapping, change management, and understanding the benefits of automation.
• Continuous support was provided through on-site sessions and detailed user manuals to mitigate resistance to change and ensure smooth integration.
Ethics Approval This study was reviewed by the Human Research Ethics Committee of Dhurakij Pundit University (DPUHREC Memorandum No. DPUHREC 0302/2567, dated February 3, 2025). The committee determined that the study did not qualify as human subjects research and was deemed exempt from further ethical review, as it involved no personal identifiers or interventions with human participants.
4 Results
The results of this study are organized into four sections: Questionnaire Survey Results, Qualitative Data Collection Results, Quantitative Data Collection Results, and Data Analysis Results. These sections provide detailed insights into the effectiveness of Robotic Process Automation (RPA) in optimizing key workflows within community pharmacies.
4.1 Questionnaire Survey Results
A structured questionnaire was completed by 120 pharmacy personnel across 12 community pharmacies. The survey gathered data on current workflow challenges, attitudes toward RPA, and readiness for automation. Tables 1 and 2 summarize the demographic data and key findings, respectively.
Table 1 Demographic data of survey respondents (N 120)
| Demographic Data | Percentage (%) |
| Gender | |
| Male | 52% |
| Female | 48% |
| Age | |
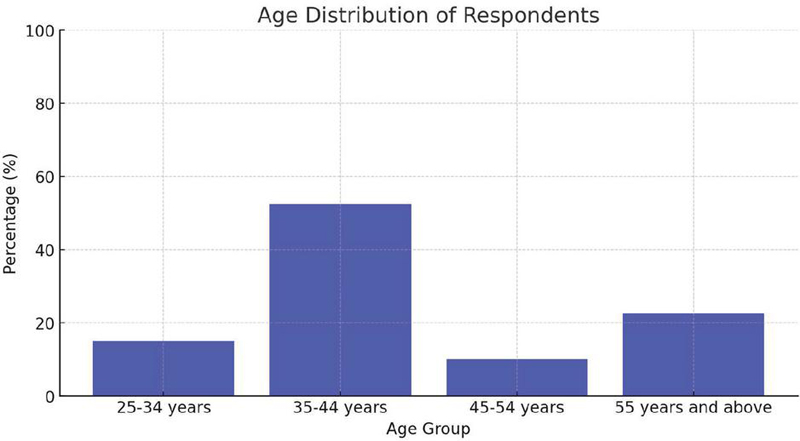
| 25–34 years | 15% |
| 35–44 years | 52.5% |
| 45–54 years | 10% |
| 55 years and above | 22.5% |
| Position in Pharmacy | |
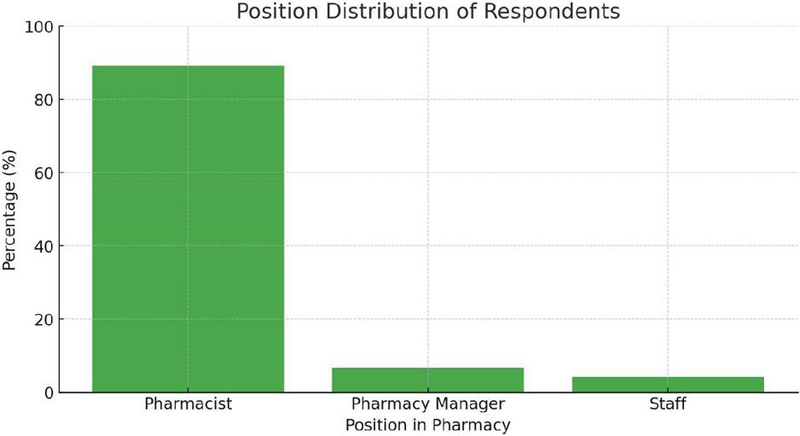
| Pharmacist | 89.2% |
| Pharmacy Manager | 6.7% |
| Staff | 4.2% |
| Experience in Pharmacy | |
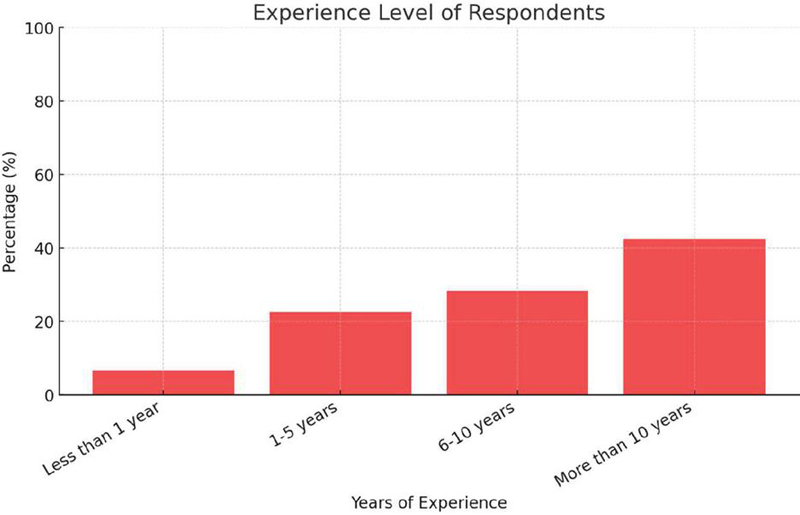
| Less than 1 year | 6.7% |
| 1–5 years | 22.5% |
| 6–10 years | 28.3% |
| More than 10 years | 42.5% |
| Type of Pharmacy | |
| Independent Pharmacy | 86.7% |
| Chain/Franchise Pharmacy | 5.8% |
| Pharmacy in Hospital | 4.2% |
| Other | 3.3% |
Table 2 Key insights from the questionnaire survey (N 120)
| Key Findings | Percentage (%) |
| Digital Readiness | |
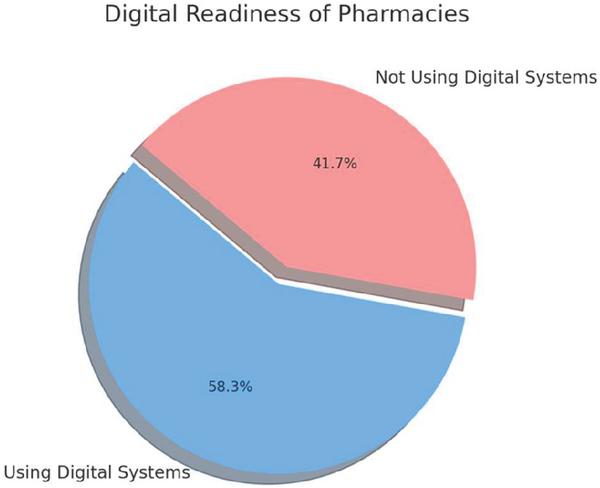
| Pharmacies using digital/automated systems | 58.30% |
| Training Needs Identified for RPA Implementation | |
| Process Mapping | 45% |
| Basic Digital Skills Training | 40.80% |
| Project Management for Technology | 35% |
| Concerns About RPA Adoption | |
| High Costs | 65% |
| Training Requirements | 55% |
| Resistance to Change | 50% |
| Readiness for RPA Implementation | |
| Ready with Proper Training and Support | 75% |
| Preferred RPA Use Cases | |
| Patient Registration and Prescription Recording | 23.30% |
| Insurance Verification and Claims Processing | 15.80% |
| Inventory Management and Stock Ordering | 11.70% |
| Report and Document Management | 11.70% |
This bar chart illustrates the distribution of respondents across different age groups. The majority of participants fall within the 35–44 age range (52.5%), followed by those aged 55 and above (22.5%). The least represented group is the 25–34 age range (15%), indicating that mid-career professionals form the largest portion of the surveyed pharmacy personnel.
Figure 1 Age distribution of respondents.
Figure 2 Position distribution of respondents.
This bar chart presents the proportion of respondents based on their roles in community pharmacies. Pharmacists constitute the largest group (89.2%), while pharmacy managers and other staff members account for smaller proportions (6.7% and 4.2%, respectively). This distribution suggests that pharmacists are the primary decision-makers and key stakeholders in RPA adoption within community pharmacies.
Figure 3 Experience level of respondents.
This bar chart illustrates the distribution of respondents based on their years of experience in pharmacy practice. The majority (42.5%) have more than 10 years of experience, while 28.3% fall within the 6–10 year range. Newer professionals, with less than 1 year of experience, represent only 6.7% of respondents. These findings highlight that a significant portion of respondents are experienced professionals, which may influence their perspectives on RPA adoption and automation in pharmacy workflows.
Figure 4 Digital readiness of pharmacies.
Digital Readiness: The survey indicates that 58.3% of pharmacies currently use some form of digital or automated system, reflecting a moderate level of technological integration and openness to further automation through RPA.
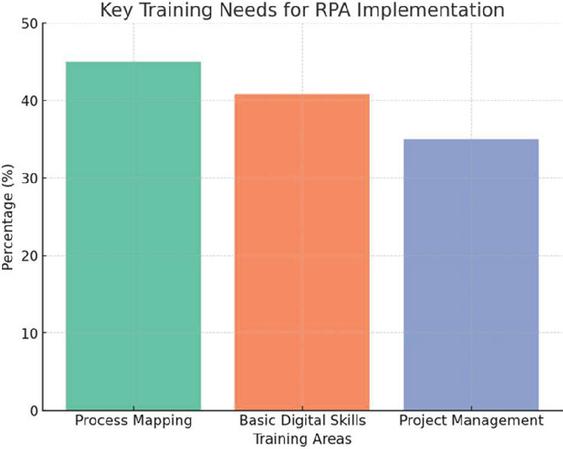
Figure 5 Key training needs for RPA implementation.
Training Needs and Concerns: Key training needs include process mapping (45%), basic digital skills (40.8%), and project management for technology (35%), which are essential for smooth RPA adoption. Concerns primarily revolve around high costs (65%), training requirements (55%), and potential resistance to change (50%).
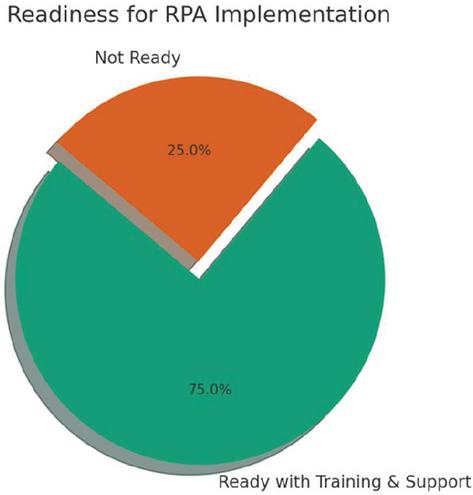
Figure 6 Readiness for RPA implementation.
Readiness for RPA Implementation: A substantial proportion (75%) of respondents expressed readiness to adopt RPA if adequate training and support are provided, showing a generally positive attitude toward automation.
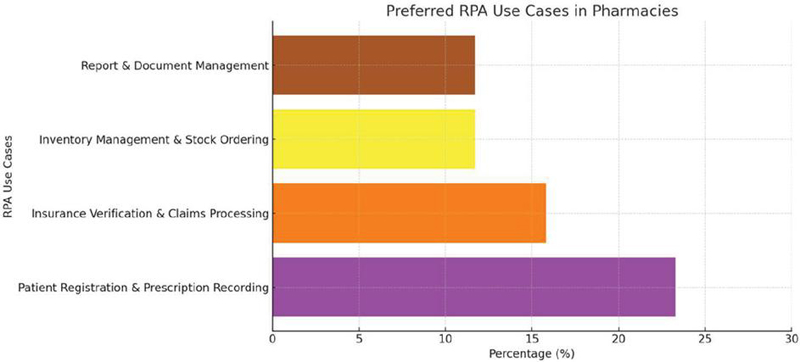
Figure 7 Preferred RPA use cases.
Preferred RPA Use Cases: Respondents identified specific pharmacy tasks that are most suitable for RPA. These include patient registration and prescription recording (23.3%), insurance verification and claims processing (15.8%), inventory management and stock ordering (11.7%), and report and document management (11.7%). This data highlights the areas where automation could most significantly improve efficiency and reduce manual workload.
4.2 Qualitative Data Collection Results
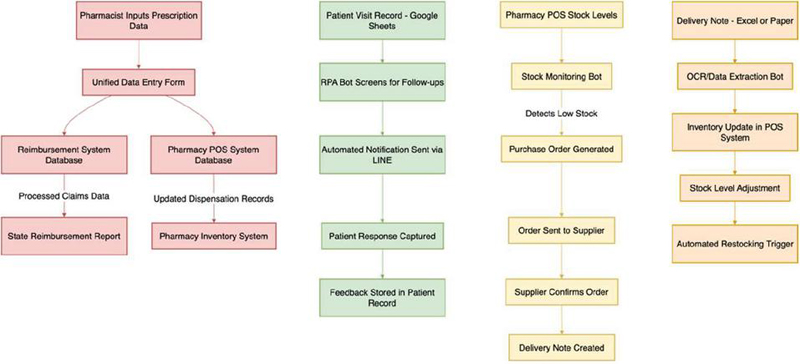
Qualitative insights were obtained through semi-structured interviews (n 15) and direct observations across the 12 selected pharmacies. A workflow diagram (see Figure 1) was also developed to visually illustrate the sequence of tasks and data flow. Key themes identified from these activities are summarized in Table 3.
Table 3 Key themes from qualitative data collection
| Theme | Description |
| Current Workflow Challenges | Manual data entry errors, repetitive administrative tasks, and time-consuming processes. |
| Expectations from RPA | Automation of prescription data entry, inventory management, and patient follow-up tasks. |
| Concerns Over RPA Adoption | Complexity, cost, integration issues with existing systems, and change management challenges. |
| Readiness for Change and Training Needs | Need for comprehensive training, user-friendly systems, and technical support. |
Interviews revealed that pharmacy personnel perceive current workflows as error-prone and labor-intensive. There is a clear demand for automation, particularly in prescription processing, inventory management, and patient follow-up, though concerns about cost and integration remain significant.
4.3 Quantitative Data Collection Results
RPA Prototypes Evaluated:
• Automated Prescription Dispensation Workflow:This prototype consolidates data entry for prescription dispensation across both the pharmacy’s POS and external state reimbursement platforms (e.g., KTB, Amed Care). It reduced duplicate data entry and processing time.
• Inventory Management Automation Workflow:Instead of relying solely on OCR (which has limitations with the Thai language), this workflow extracts delivery data from an Excel file and automates its entry into the POS system, significantly reducing manual data entry time and errors.
• Patient Follow-up and Alerts Workflow:Leveraging data from a Google Sheet, this RPA bot screens patients due for follow-up, sends automated notifications via LINE, and captures patient feedback. This automation reduced follow-up time and increased patient engagement.
• Automated Medication Ordering Workflow:This solution continuously monitors stock levels and, upon reaching a reorder threshold, automatically generates and sends purchase orders via email to suppliers, ensuring optimal inventory levels.
Table 4 Key outcomes from RPA prototypes
| RPA Prototype | Outcome | Improvement (%) |
| Automated Prescription Dispensation | Reduced duplicate data entry and streamlined data processing; processing time reduced from 15 to 5 minutes. | 67% time reduction |
| Inventory Management Automation | Automated data transfer from Excel to POS; reduced data entry time from 25 to 10 minutes. | 60% time reduction |
| Patient Follow-up and Alerts | Automated notifications reduced follow-up time from 40 to 8 minutes; patient engagement increased from 60% to 100% (66.7% increase). | 80% time reduction; 66.7% engagement increase |
| Automated Medication Ordering | Automated stock monitoring and purchase order generation; ordering time reduced from 60 to 10 minutes. | 83% time reduction |
Table 4 summarizes the key outcomes of deploying Robotic Process Automation (RPA) prototypes in four prioritized pharmacy workflows. Each RPA solution was designed to address specific workflow challenges, streamline operations, and improve efficiency. The table provides an overview of the measurable improvements observed in terms of time savings, error reduction, and enhanced engagement. Here’s a breakdown of each RPA prototype and its outcomes:
1. Automated Prescription Dispensation:
∘ This RPA prototype focuses on reducing duplicate data entry tasks by integrating data entry processes across both the external state reimbursement platforms and the pharmacy’s Point of Sale (POS) system. As a result, it significantly reduced the average time required for prescription dispensation recording by 67% and decreased the error rate by 83%. These improvements reflect more streamlined workflows and enhanced data accuracy, which reduces the administrative burden on pharmacists and allows them to focus more on patient
| Time Reduction |
2. Inventory Management Automation:
∘ The RPA solution for inventory management involved automating the data transfer process from Excel-based delivery notes into the pharmacy’s POS system, thereby eliminating manual data entry. This led to a substantial 60% reduction in the time required for inventory updates and a 93% reduction in data entry errors. These outcomes demonstrate the effectiveness of RPA in improving the accuracy and speed of inventory management processes, which is crucial for maintaining optimal stock levels and ensuring medication availability.
| Time Reduction |
3. Patient Follow-up and Alerts:
∘ This prototype uses RPA to automate the follow-up process for patients after medication dispensation. It leverages patient visit data and follow-up dates recorded in Google Sheets to send automated notifications through LINE and capture patient feedback. The implementation resulted in an 80% reduction in time spent on manual follow-up tasks and a 40% increase in patient engagement rates. This shows that RPA can effectively enhance patient communication and follow-up efficiency, leading to better patient outcomes and satisfaction.
| Follow-up Time Reduction |
4. Automated Medication Ordering:
∘ The RPA for medication ordering automates the process of generating reports on current monthly stock levels and usage. It extracts data on medications with negative stock levels and creates a purchase order, which is then sent to the medicine supplier through LINE. This automation reduced the time spent on ordering by 83%. By streamlining the medication ordering process, pharmacies can prevent stockouts, maintain adequate inventory, and minimize medication shortages, thus ensuring continuous and effective service delivery.
| Ordering Time Reduction |
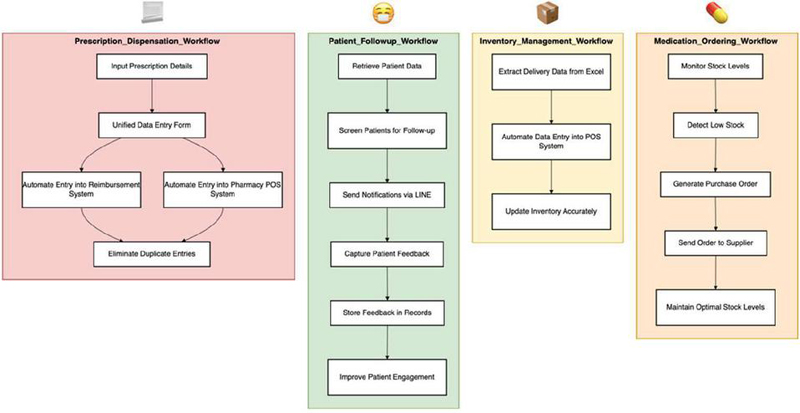
Figure 8 The workflow diagram illustrate the sequence of tasks for each RPA solution and the corresponding data flow.
Figure 9 The data flow diagram, Inventory Management, Patient Follow-up, and Medication Ordering.
The data flow diagram illustrates how information is processed and transmitted within the Robotic Process Automation (RPA) system implemented in community pharmacies. The diagram is divided into four key sections, each representing a critical pharmacy workflow automated using RPA: Prescription Dispensation
4.4 Data Analysis Results
Descriptive statistics and inferential analyses were employed to evaluate the effectiveness of RPA implementations. Quantitative data, such as processing times, error counts, and patient engagement rates, were measured before and after RPA deployment. All measurements are in minutes, with patient engagement reported as a percentage.
Paired sample t-tests were conducted to assess the statistical significance of differences between manual workflows and those optimized with RPA. Table 5 summarizes these results.
Table 5 Summary of paired sample t-test results for RPA implementation in pharmacy workflows
| Workflow | ||||||
| Activity | Metric | Before RPA (Mean SD) | After RPA (Mean SD) | Mean Difference | t-Statistic | p-Value |
| Automated Prescription Dispensation | Processing Time (minutes) | 15.0 4.5 | 5.0 1.8 | -10 | 9.23 | 0.001 |
| Task Duplication Reduction (instances) | 2.5 0.9 | 0.5 0.2 | -2 | 8.75 | 0.001 | |
| Inventory Management Automation | Data Entry Time (minutes) | 25.0 7.1 | 10.0 3.6 | -15 | 7.89 | 0.001 |
| Manual Entry Count (entries) | 20.0 6.4 | 3.0 1.0 | -17 | 11.25 | 0.001 | |
| Patient Follow-up and Alerts | Patient Engagement Rate (%) | 60.0 10.2 | 100.0 5.0 | 40 | 6.67 | 0.001 |
| Follow-up Time (minutes) | 40.0 8.5 | 8.0 3.2 | -32 | 11.34 | 0.001 | |
| Automated Medication Ordering | Ordering Time (minutes) | 60.0 15.0 | 10.0 2.8 | -50 | 9.02 | 0.001 |
| Report Generation Time (minutes) | 30.0 7.5 | 5.0 1.5 | -25 | 10.18 | 0.001 |
The paired sample t-tests were conducted to evaluate the effectiveness of RPA implementations across four key pharmacy workflows: Automated Prescription Dispensation, Inventory Management Automation, Patient Follow-up and Alerts, and Automated Medication Ordering. Each workflow activity was tested multiple times (10 observations per workflow) to ensure robust and reliable results.
The tests showed statistically significant improvements across all measured metrics after RPA implementation. Notably, the time required for tasks such as prescription dispensation, inventory data entry, patient follow-up, and medication ordering was significantly reduced. For example, prescription dispensation processing time decreased from 15 minutes to 5 minutes per transaction, and patient follow-up time was reduced from 40 minutes to 8 minutes. Similarly, manual task duplication, data entry counts, and report generation times also saw significant reductions. These results highlight the substantial efficiency gains and workload reduction that RPA can provide in community pharmacy settings.
5 Discussions
The findings from this study demonstrate the transformative potential of Robotic Process Automation (RPA) in optimizing workflows within community pharmacies. By automating repetitive and time-consuming tasks, RPA not only enhances operational efficiency and reduces manual workload but also improves service quality. This discussion synthesizes the quantitative results, qualitative insights, and survey data to present a comprehensive view of both the technological and human aspects of RPA adoption.
5.1 Impact of RPA on Pharmacy Operations
Quantitative results indicate substantial improvements following RPA implementation. For instance, the automated prescription dispensation workflow reduced processing time by 67% (from 15 minutes to 5 minutes per transaction), while the automated medication ordering process achieved an 83% reduction in ordering time (from 60 minutes to 10 minutes per order). Similarly, the patient follow-up workflow reduced manual follow-up time by 80% (from 40 minutes to 8 minutes per follow-up), and patient engagement increased by 66.7%. These significant improvements confirm that RPA can effectively decrease time spent on repetitive tasks, thereby allowing pharmacy staff to focus more on patient-centered activities rather than administrative duties.
These results align with the findings of Wetsiri and Paireekreng (2024), who reported a 42.86% efficiency improvement in price comparison processes via RPA in community pharmacies. Their study showed that automation not only saves time but also reduces human errors, leading to improved inventory management and enhanced financial performance [27].
5.2 Perceptions, Readiness, and Human Factors
The questionnaire survey results indicate a generally positive attitude toward RPA adoption among pharmacy personnel, with 78% of respondents believing that RPA can enhance efficiency. However, significant concerns remain regarding implementation costs (68%), training needs (54%), and potential resistance to change (50%). Notably, 75% of respondents expressed readiness to adopt RPA provided that adequate training and support are in place. The qualitative interviews further underscore these points, highlighting challenges related to the complexity of RPA systems and difficulties integrating them with existing pharmacy management platforms. This combined evidence suggests that, although there is strong enthusiasm for RPA, successful implementation will depend heavily on proper education, targeted training programs, and effective communication about the benefits and ease of use of these systems.
5.3 Challenges and Considerations in Implementation
Despite the clear benefits, several challenges persist:
• System Integration: One of the most significant hurdles is integrating RPA with existing pharmacy management systems. Achieving seamless integration requires effective change management strategies, including phased implementation and continuous training.
• Financial Investment: Cost remains a major barrier, particularly for smaller, independent pharmacies, as 68% of respondents cited financial constraints. Leveraging cost-effective solutions such as low-code/no-code platforms (e.g., Microsoft Power Automate) can help mitigate these challenges.
• Change Management: Resistance to change, reported by 50% of respondents, underscores the need for strategic stakeholder engagement. Involving all levels of pharmacy personnel in the decision-making process and clearly communicating the benefits of RPA can help ease the transition.
5.4 Implications for Pharmacy Practice and Future Research
The successful implementation of RPA in community pharmacies has broad implications for pharmacy practice. Automating routine and repetitive tasks not only enhances operational efficiency but also allows pharmacy staff to shift focus towards more value-added services, such as patient counselling and health management. This shift can help redefine the role of pharmacists from mere dispensers to more holistic healthcare providers, ultimately improving patient outcomes and increasing pharmacy revenue through diversified service offerings.
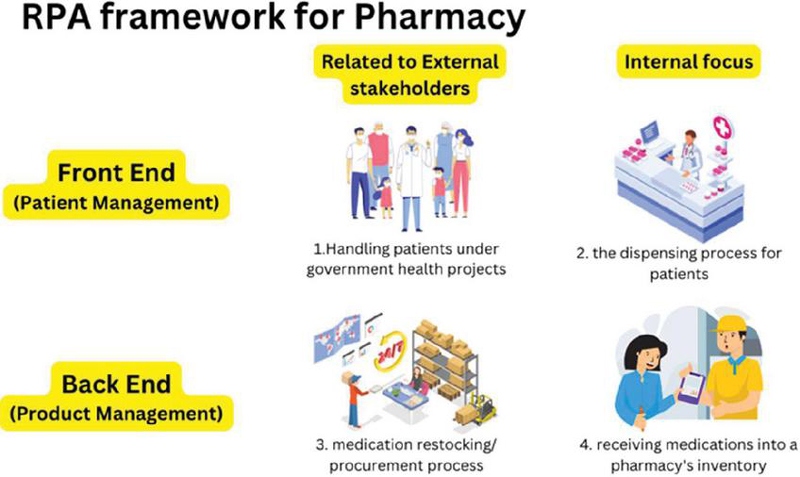
Figure 10 RPA framework for pharmacy.
The findings of this study align with those presented by Soprakan and Kiattisin (2021), who explored the impact of disruptive technologies like RPA on Sustainable Enterprise Resource Planning (S-ERP). Their research demonstrated that integrating RPA with existing ERP systems can lead to substantial time savings and financial benefits, such as a 52% Internal Rate of Return (IRR) and a payback period of 3.6 years. These results underscore the strategic advantages of RPA beyond healthcare settings, highlighting its potential to enhance business process efficiency and sustainability in various industries [28].
By extending the concept of RPA integration to community pharmacies, it becomes evident that pharmacies can leverage this technology to not only streamline operational processes but also contribute to broader sustainability goals, similar to the benefits seen in enterprise systems. Future research could explore the applicability of these findings in diverse pharmacy settings, examining how RPA can be used to optimize resource utilization, reduce environmental impact, and improve long-term operational sustainability.
The successful outcomes of RPA in both pharmacy operations and enterprise systems suggest a convergence of healthcare and business process management technologies. This intersection points to an opportunity for cross-industry learning and the development of integrated solutions that address both operational efficiency and strategic sustainability goals. Further studies could investigate the potential for developing standardized RPA frameworks that cater to the unique needs of different sectors while promoting shared objectives like efficiency, cost reduction, and sustainable development.
Future research should explore the long-term impact of RPA on pharmacy practice, especially concerning patient satisfaction and outcomes. Additionally, studies should examine the scalability of RPA solutions across various pharmacy settings – from small independent stores to larger chain pharmacies and hospital environments. Understanding the variations in RPA effectiveness across different contexts can provide valuable insights for tailoring implementation strategies and maximizing the benefits of automation.
5.5 Suggested Approach for Measuring Improvements
To better understand the impact of RPA on pharmacy workflows, the following approaches are recommended for measuring improvements effectively:
• Time-Based Metrics: For metrics like time reduction, ensure consistent measurement before and after RPA implementation. Use time logs, POS system records, or manual stopwatch timing to calculate the exact duration of tasks.
• Engagement and Adherence Metrics: Patient engagement improvements can be measured by tracking response rates to automated notifications versus manual follow-ups.
• Data Collection Period: Ensure that the data collection period is sufficient to observe meaningful changes. For example, time reductions can typically be observed immediately, while improvements in engagement or error rates might need a few weeks or months of data collection.
5.6 Recommendations for Successful RPA Implementation
Based on the study findings, several recommendations can be made to facilitate successful RPA implementation in community pharmacies:
• Comprehensive Training and Support: Adequate training is crucial for pharmacy staff to understand and effectively use RPA systems. Providing hands-on training sessions and user-friendly manuals can help reduce apprehension and improve confidence in using new technology.
• Phased Implementation Approach: Implementing RPA in phases, starting with simpler tasks such as inventory management before moving to more complex processes, can help pharmacies gradually adapt to the new systems without overwhelming staff.
• Integration with Existing Systems: Ensuring that RPA solutions are compatible with existing pharmacy management systems is essential for smooth integration. Collaborating with technology vendors to customize solutions to the specific needs of each pharmacy can minimize disruptions during the transition.
• Stakeholder Engagement: Engaging all stakeholders, including pharmacy owners, pharmacists, and support staff, in the decision-making process can help build consensus and foster a positive attitude toward change.
• Monitoring and Continuous Improvement: Regular monitoring of RPA performance and collecting feedback from users can help identify areas for improvement and ensure that the systems remain efficient and relevant to evolving pharmacy needs.
6 Conclusions
This study confirms that Robotic Process Automation (RPA) can significantly optimize operations in community pharmacies by reducing manual workload, enhancing efficiency, and improving data accuracy and patient engagement. The measurable improvements – such as a 67% reduction in prescription dispensation time and an 83% reduction in medication ordering time – underscore the immediate benefits of automating routine, labor-intensive tasks.
Key Findings:
• Efficiency Gains: RPA dramatically reduces task completion times, allowing pharmacy staff to reallocate time toward patient-centered activities.
• Error Reduction and Data Accuracy: Qualitative insights suggest that automating data entry can minimize errors and consolidate information across systems.
• Positive Perceptions and Readiness: A majority of respondents recognize the potential of RPA and are willing to adopt it, provided that adequate training and support are in place.
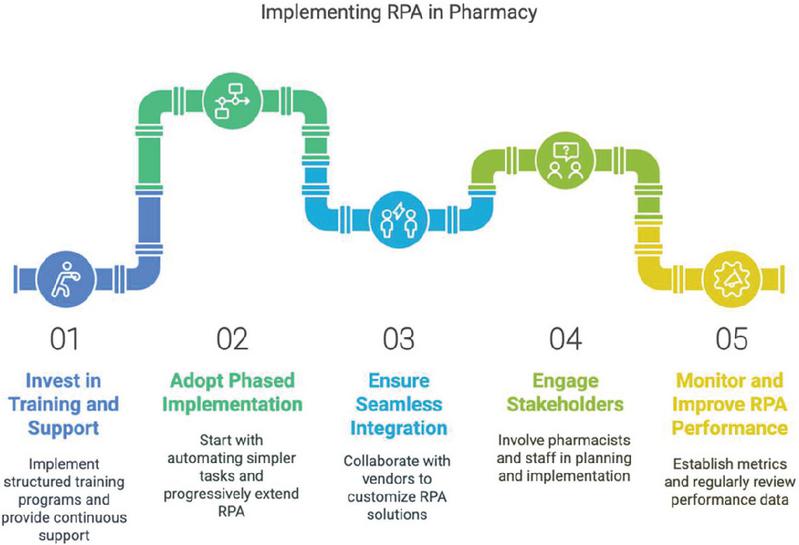
Figure 11 RPA implementation framework for community pharmacies.
• Implementation Challenges: Despite the benefits, challenges such as integration complexity, high financial investment, and resistance to change persist.
Practical Recommendations for Pharmacy Practitioners:
1. Invest in Comprehensive Training and Support:
∘ Implement structured training programs that cover both the technical use of RPA tools and process re-engineering.
∘ Provide continuous on-site support and user-friendly manuals to ease the transition.
2. Adopt a Phased Implementation Strategy:
∘ Start with automating simpler, low-risk tasks (e.g., inventory management) and progressively extend RPA to more complex processes.
∘ This phased approach minimizes disruption and allows staff to gradually adapt to the new systems.
3. Ensure Seamless Integration with Existing Systems:
∘ Collaborate closely with technology vendors to customize RPA solutions that align with existing pharmacy management systems.
∘ Prioritize systems that are cost-effective (such as low-code/no-code platforms) to reduce financial barriers.
4. Engage Stakeholders Throughout the Process:
∘ Involve pharmacists, managers, and support staff in every stage of the planning and implementation.
∘ Transparent communication about the benefits and ease of use of RPA can help overcome resistance to change.
5. Monitor and Continuously Improve RPA Performance:
∘ Establish clear performance metrics (e.g., time reduction in minutes per transaction, error rates, patient engagement percentages).
∘ Regularly review performance data to identify opportunities for further improvement and to ensure long-term sustainability.
Future Research Directions: Further studies should explore the long-term impacts of RPA on error reduction, patient satisfaction, and overall pharmacy performance. Research should also focus on the scalability of RPA solutions across various pharmacy settings – from small independent stores to larger chains and hospital pharmacies – and on developing standardized frameworks that address both technical challenges and human factors.
In conclusion, RPA holds substantial promise for transforming community pharmacy operations. By following the recommendations above and addressing the identified challenges, pharmacy practitioners can maximize the benefits of automation, ultimately leading to improved service quality and enhanced patient care.
Acknowledgment
We sincerely thank all the pharmacy owners, pharmacists, and staff who participated in this study. Their invaluable insights and cooperation were crucial in understanding the current workflows and challenges faced in community pharmacies, providing a solid foundation for this research.
We also wish to acknowledge the development of the RPA prototypes in this study, created using Microsoft Power Automate Desktop. The design, implementation, and testing of these automation solutions were conducted by the research team, demonstrating the potential of low-code/no-code platforms in streamlining pharmacy operations.
Lastly, we express our gratitude to our colleagues and institutions for their continuous support, guidance, and encouragement throughout this research process. Their contributions have been instrumental in the successful completion of this study.
References
[1] Hofmann, P., Samp, C., and Urbach, N. (2019). Robotic process automation. Electronic Markets, 30(1), 99-106. https://doi.org/10.1007/s12525-019-00365-8.
[2] Smeets, M., Erhard, R., and Kaußler, T. (2021). Success Factors of RPA Implementations. Robotic Process Automation (RPA) in the Financial Sector. https://doi.org/10.1007/978-3-658-32974-7\_7.
[3] Costa, D., Mamede, H., and Silva, M. (2022). Robotic Process Automation (RPA) Adoption: A Systematic Literature Review. Engineering Management in Production and Services, 14, 1–12. https://doi.org/10.2478/emj-2022-0012.
[4] Herm, L., Janiesch, C., Helm, A., Imgrund, F., Fuchs, K., Hofmann, A., and Winkelmann, A. (2020). A Consolidated Framework for Implementing Robotic Process Automation Projects. EMISA Forum, 41, 15–16. https://doi.org/10.1007/978-3-030-58666-9\_27.
[5] Leno, V., Polyvyanyy, A., Dumas, M., Rosa, M., and Maggi, F. (2020). Robotic process mining: Vision and challenges. Business & Information Systems Engineering, 1–14. https://doi.org/10.1007/s12599-020-00641-4.
[6] Yadav, N., and Panda, S. (2022). A Path Forward for Automation in Robotic Process Automation Projects: Potential Process Selection Strategies. 2022 International Conference on Machine Learning, Big Data, Cloud and Parallel Computing (COM-IT-CON), 1, 801–805. https://doi.org/10.1109/com-it-con54601.2022.9850739.
[7] Bahaweres, R., Amna, H., and Nurnaningsih, D. (2022). Improving Purchase to Pay Process Efficiency with RPA using Fuzzy Miner Algorithm in Process Mining. 2022 International Conference on Decision Aid Sciences and Applications (DASA), 1483–1488. https://doi.org/10.1109/DASA54658.2022.9765091.
[8] Wewerka, J., and Reichert, M. (2021). Checklist-based Support of Knowledge Workers in Robotic Process Automation Projects. 2021 IEEE 23rd Conference on Business Informatics (CBI), 01, 52–61. https://doi.org/10.1109/CBI52690.2021.00016.
[9] Piyatilake, A., Thibbotuwawa, A., and Silva, M. (2022). RPA success remains a non-trivial endeavor. Bolgoda Plains. https://doi.org/10.31705/bprm.v2(1).2022.12.
[10] Nielsen, I., Piyatilake, A., Thibbotuwawa, A., Silva, M., Bocewicz, G., and Banaszak, Z. (2023). Benefits Realization of Robotic Process Automation (RPA) Initiatives in Supply Chains. IEEE Access, 11, 37623–37636. https://doi.org/10.1109/ACCESS.2023.3266293.
[11] NHS Transformation Directorate, and Atos. (2022). RPA in the NHS: Guidance for designing, delivering and sustaining RPA within the NHS. Retrieved from https://transform.england.nhs.uk/media/documents/RPA-Guidance-May-22.pdf.
[12] Radke, A., Dang, M., and Tan, A. (2020). Using robotic process automation (RPA) to enhance item master data maintenance process. Logforum. https://doi.org/10.17270/J.LOG.2020.380.
[13] Sumathi, N., and Jeyalakshmi, A. (2022). Implementing robotic process automation to improve operational efficiency in the health-care sector. International journal of health sciences. https://doi.org/10.53730/ijhs.v6ns1.7256.
[14] Baumann, A., and Cabassa, L. (2020). Reframing implementation science to address inequities in healthcare delivery. BMC Health Services Research, 20. https://doi.org/10.1186/s12913-020-4975-3.
[15] Ministry of Public Health of Thailand. (2014). Good Pharmacy Practice (GPP) guidelines Bureau of Drug Control, Food and Drug Administration (FDA), Thailand, 2014. [Online]. Available: https://drug.fda.moph.go.th/media.php?id=543001067651211264\&name=GPP\_Guideline\_final29Oct2015.pdf. [Accessed: Sep. 10, 2024].
[16] Bou-Saba, A., Kassak, K., and Salameh, P. (2023). Adherence to Good Pharmacy Practices by Community Pharmacies in Lebanon and Opportunities for Quality Improvement: It is Time to Act. Integrated Pharmacy Research & Practice, 12, 25–35. https://doi.org/10.2147/IPRP.S377635.
[17] Singu, B., Mutsambiwa, P., and Mvula, E. (2023). Outcomes of pharmacy facility inspections: implications on pharmaceutical services. Journal of Pharmaceutical Health Services Research. https://doi.org/10.1093/jphsr/rmad047.
[18] Punturungsee, P., and Ploylearmsang, C. (2023). Empowerment interventions for pharmacies to comply with the Good Pharmacy Practice (GPP) in Thailand. Pharmacy Practice. https://doi.org/10.18549/pharmpract.2023.3.2852.
[19] Quille, R., Almeida, F., Borycz, J., Corrêa, P., Filgueiras, L., Machicao, J., Almeida, G., Midorikawa, E., Demuner, V., Bedoya, J., and Vajgel, B. (2023). Performance analysis method for robotic process automation. Sustainability, 15(4), 3702. https://doi.org/10.3390/su15043702.
[20] Khrystolubova, N., Bailey, R., Orr, R., Gordan, L., and Auger, T. (2022). Defining appropriate quality performance metrics for pharmacies dispensing oral oncology therapies. The American journal of managed care, 28 6 Spec No., SP316–SP323. https://doi.org/10.37765/ajmc.2022.89209.
[21] Urick, B., Pathak, S., Hughes, T., and Ferreri, S. (2021). Design and effect of performance-based pharmacy payment models. Journal of Managed Care & Specialty Pharmacy, 27. https://doi.org/10.18553/jmcp.2021.27.3.306.
[22] AlQudah, A., Al-Emran, M., and Shaalan, K. (2021). Technology Acceptance in Healthcare: A Systematic Review. Applied Sciences. https://doi.org/10.3390/app112210537.
[23] J. W. Dearing and J. G. Cox, “Diffusion Of Innovations Theory, Principles, And Practice,” Health Affairs, vol. 37, no. 2, pp. 183–190, 2018. https://doi.org/10.1377/hlthaff.2017.1104.
[24] Rouidi, M., Elouadi, A., and Hamdoune, A. (2022). Acceptance and use of telemedicine technology by health professionals: Development of a conceptual model. Digital Health, 8. https://doi.org/10.1177/20552076221081693.
[25] Dhagarra, D., Goswami, M., and Kumar, G. (2020). Impact of Trust and Privacy Concerns on Technology Acceptance in Healthcare: An Indian Perspective. International Journal of Medical Informatics, 141, 104164–104164. https://doi.org/10.1016/j.ijmedinf.2020.104164.
[26] Ma, Y., and Luo, M. (2022). Older people’s intention to use medical apps during the COVID-19 pandemic in China: an application of the Unified Theory of Acceptance and Use of Technology (UTAUT) model and the Technology of Acceptance Model (TAM). Ageing and Society. https://doi.org/10.1017/s0144686x22000423.
[27] W. Wetsiri and W. Paireekreng, “Enhancing Operational Efficiency in Community Pharmacies through Robotic Process Automation,” 2024 5th Technology Innovation Management and Engineering Science International Conference (TIMES-iCON), Bangkok, Thailand, 2024, pp. 1–6, https://doi.org/10.1109/TIMES-iCON61890.2024.10630746.
[28] Soprakan, C., and Kiattisin, S. (2021). Impact of Disruptive Technology on Sustainable Enterprise Resource Planning (S-ERP). Journal of Mobile Multimedia, 17(4),749–772. https://doi.org/10.13052/jmm1550-4646.17413.
Biographies

Wirun Wetsiri is currently pursuing his studies at the College of Innovative Technology and Engineering, Dhurakij Pundit University in Bangkok, Thailand. His research interests focus on robotic process automation, workflow optimization, and the application of automation technologies in healthcare settings, particularly in community pharmacies.

Worapat Paireekreng, Ph.D., received his Ph.D. in Information Technology from Murdoch University, Australia, in 2013. He earned his M.Sc. in Information System Management with honors from the National Institute of Development Administration (NIDA) in 2000 and his B.B.A. in Management Information Systems from Thammasat University in 1997. He is currently a faculty member at King Mongkut’s Institute of Technology Ladkrabang, Bangkok, Thailand. His research areas include data mining, data analytics, information technology, and its applications. He has published numerous research articles in both national and international journals.
Journal of Mobile Multimedia, Vol. 21_1, 113–148.
doi: 10.13052/jmm1550-4646.2115
© 2025 River Publishers