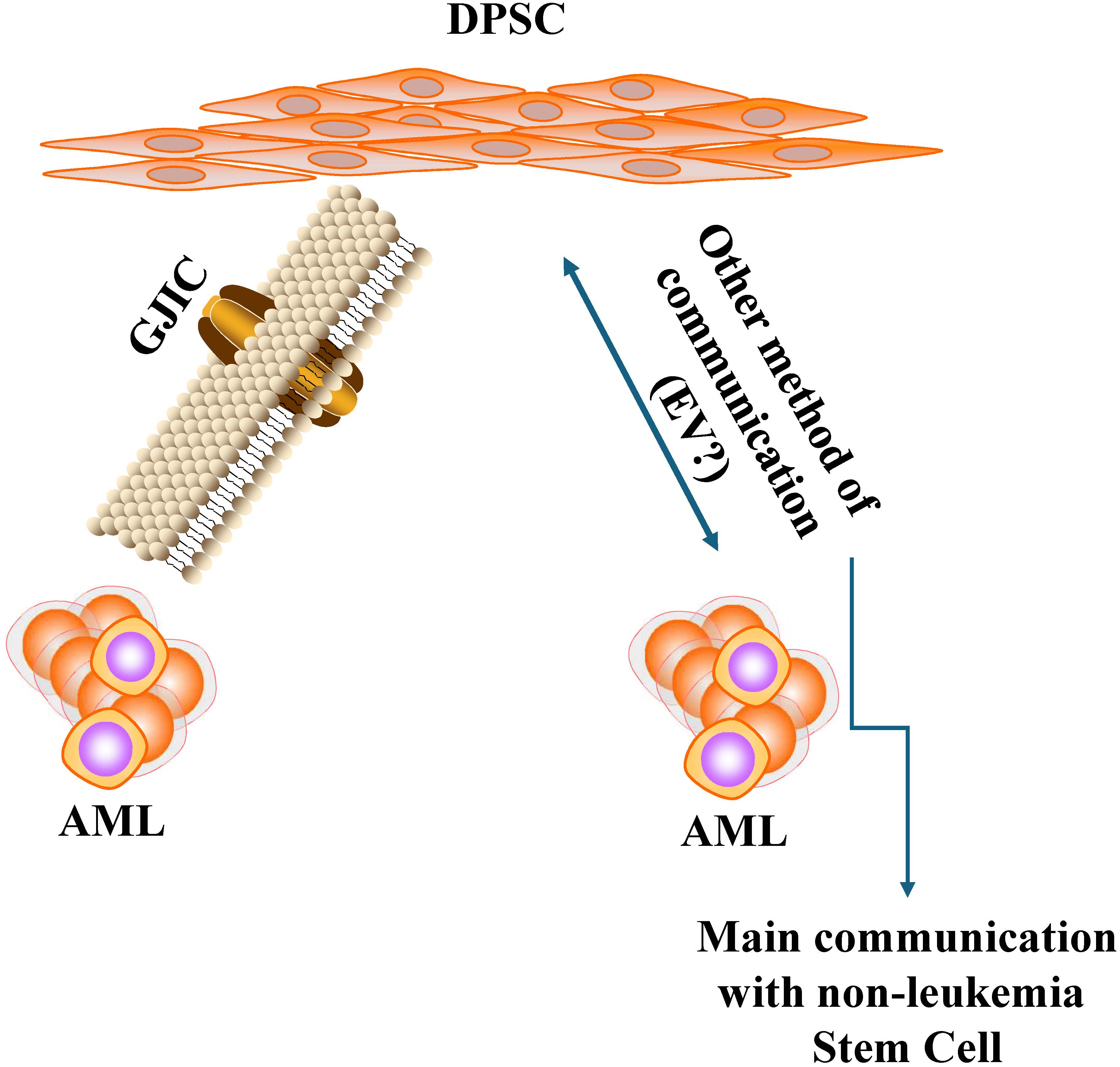
Intercellular Interaction Between a Dental Pulp Stem Cell and Leukemia Cells – Support of Acute Myeloid Leukemia
DOI:
https://doi.org/10.13052/ijts2246-8765.2025.005Keywords:
Leukemia, stem cell, dental pulp, gap junctionAbstract
The oral cavity is a site of hematopoietic activity, and metastatic hematological and solid tumors. This study focused on acute myeloid leukemia (AML) due to extensive documentation of its presentation in the gingiva. Despite these reports, it is unclear how AML and other leukemia cells survive in the oral tissue. We investigated intercellular communication between leukemia cells and dental pulp stem cells (DPSCs). DPSCs enhanced the proliferation and adhesion of AML cells (HL-60) and to a lesser extent, myelomoncytic leukemia cells (U937). The erythroleukemia K562 cells showed a delayed trend to proliferate. The communication between DPSCs and HL-60 cells was partly due to gap junctional intercellular communication (GJIC), as indicated by dye transfer. We also noted evidence of tunnelling nanotubules (TNT). Dye transfer was noted in non-adherent cells, suggesting other method of transfer, perhaps by extracellular vesicles. Using SORE-6 that can stratify the HL-60 subset, dye transfer occurred mostly in the subset lowest in the hierarchy. These latter findings were novel since they might provide insights into the behavior of non-leukemia stem cells and their interaction with cells in the oral cavity. In summary, this study began to dissect the interaction between HL-60 AML cells and DPSCs, providing insights into the survival of AML and perhaps other leukemia cells in the oral cavity.
Downloads
References
Janowiak-Majeranowska, A., J. Osowski, B. Mikaszewski, and A. Majeranowski. 2022. Secondary oral cancer after systemic treatment of hematological malignancies and oral GVHD: a systematic review. Cancers 14: 2175.
Hirshberg, A., A. Shnaiderman-Shapiro, I. Kaplan, and R. Berger. 2008. Metastatic tumours to the oral cavity - pathogenesis and analysis of 673 cases. Oral Oncol 44: 743–752.
Anderson, L. J., M. Girguis, E. Kim, J. Shewale, M. Braunlin, W. Werther, J. E. Hidalgo-Lopez, F. Zaman, and C. Kim. 2024. A temporal and multinational assessment of acute myeloid leukemia (AML) cancer incidence, survival, and disease burden. Leuk Lymphoma: 1–10.
Gopal, S., K. P. Shetty, V. Jindal, and M. Saritha. 2011. Interrelationship of Endodontic-Periodontal Lesions-An Overview. Indian J Dental Sci 3.
Bruno, K. F., F. B. Barletta, W. T. Felippe, J. A. Silva, A. H. G. de Alencar, and C. Estrela. 2014. Oxygen saturation in the dental pulp of permanent teeth: a critical review. Journal of endodontics 40: 1054–1057.
Fernandes, K. S., M. Gallottini, T. Castro, M. F. Amato, J. S. Lago, and P. H. Braz-Silva. 2018. Gingival leukemic infiltration as the first manifestation of acute myeloid leukemia. Special Care in Dentistry 38: 160–162.
Sonoi, N., Y. Soga, H. Maeda, K. Ichimura, T. Yoshino, K. Aoyama, N. Fujii, Y. Maeda, M. Tanimoto, R. Logan, J. Raber-Durlacher, and S. Takashiba. 2012. Histological and immunohistochemical features of gingival enlargement in a patient with AML. Odontology 100: 254–257.
Shankarapillai, R., M. A. Nair, R. George, and L. J. Walsh. 2010. Periodontal and gingival parameters in young adults with acute myeloid leukaemia in Kerala, South India. Oral Health Prev Dent 8: 395–400.
Gallipoli, P., and M. Leach. 2007. Gingival infiltration in acute monoblastic leukaemia. Br Dent J 203: 507–509.
Demirer, S., H. Ozdemir, M. Sencan, and I. Marakoglu. 2007. Gingival hyperplasia as an early diagnostic oral manifestation in acute monocytic leukemia: a case report. Eur J Dent 1: 111–114.
Cooper, C. L., R. Loewen, and T. Shore. 2000. Gingival hyperplasia complicating acute myelomonocytic leukemia. J Can Dent Assoc 66: 78–79.
Hasan, S., N. I. Khan, and L. B. Reddy. 2015. Leukemic gingival enlargement: Report of a rare case with review of literature. Int J Appl Basic Med Res 5: 65–67.
Hou, G. L., and C. C. Tsai. 1988. Primary gingival enlargement as a diagnostic indicator in acute myelomonocytic leukemia. A case report. J Periodontol 59: 852–855.
Arnold, M., E. Morgan, H. Rumgay, A. Mafra, D. Singh, M. Laversanne, J. Vignat, J. R. Gralow, F. Cardoso, and S. Siesling. 2022. Current and future burden of breast cancer: Global statistics for 2020 and 2040. The Breast 66: 15–23.
Cammarata-Scalisi, F., K. Girardi, L. Strocchio, P. Merli, A. Garret-Bernardin, A. Galeotti, F. Magliarditi, A. Inserra, and M. Callea. 2020. Oral Manifestations and Complications in Childhood Acute Myeloid Leukemia. Cancers (Basel) 12.
Dreizen, S., K. B. McCredie, M. J. Keating, and M. A. Luna. 1983. Malignant gingival and skin “infiltrates” in adult leukemia. Oral Surg Oral Med Oral Pathol 55: 572–579.
Pugh, C. W., and P. J. Ratcliffe. 2003. Regulation of angiogenesis by hypoxia: role of the HIF system. Nat Med 9: 677–684.
Forte, D., M. García-Fernández, A. Sánchez-Aguilera, V. Stavropoulou, C. Fielding, D. Martín-Pérez, J. A. López, A. S. H. Costa, L. Tronci, E. Nikitopoulou, M. Barber, P. Gallipoli, L. Marando, C. L. Fernández de Castillejo, A. Tzankov, S. Dietmann, M. Cavo, L. Catani, A. Curti, J. Vázquez, C. Frezza, B. J. Huntly, J. Schwaller, and S. Méndez-Ferrer. 2020. Bone Marrow Mesenchymal Stem Cells Support Acute Myeloid Leukemia Bioenergetics and Enhance Antioxidant Defense and Escape from Chemotherapy. Cell Metab 32: 829–843.e829.
Williams WJ, B. E., Erslev AJ, Lichtman MA. 1990. Hematology. 4th ed. M. Hill, ed, New York. 243–244.
Felix, D. E., and J. Lukens. 1986. Oral symptoms as a chief sign of acute monoblastic leukemia: report of case. J Am Dent Assoc 113: 899–900.
Brenneise, C. V., J. S. Mattson, and J. R. Commers. 1988. Acute myelomonocytic leukemia with oral manifestations: report of case. J Am Dent Assoc 117: 835–837.
Epstein, J. B., R. W. Priddy, T. Sparling, and L. Wadsworth. 1986. Oral manifestations in myelodysplastic syndrome. Review of the literature and report of a case. Oral Surg Oral Med Oral Pathol 61: 466–470.
Khera, P., M. J. Zirwas, and J. C. English, 3rd. 2005. Diffuse gingival enlargement. J Am Acad Dermatol 52: 491–499.
Pogrel, M. A. 1978. Acute leukemia. An atypical case presenting with gingival manifestations. Int J Oral Surg 7: 119–122.
McKenna, S. J. 2000. Leukemia. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 89: 137–139.
Wu, J., J. E. Fantasia, and R. Kaplan. 2002. Oral manifestations of acute myelomonocytic leukemia: a case report and review of the classification of leukemias. J Periodontol 73: 664–668.
Elad, S., J. E. Raber-Durlacher, M. T. Brennan, D. P. Saunders, A. P. Mank, Y. Zadik, B. Quinn, J. B. Epstein, N. M. Blijlevens, and T. Waltimo. 2015. Basic oral care for hematology–oncology patients and hematopoietic stem cell transplantation recipients: a position paper from the joint task force of the Multinational Association of Supportive Care in Cancer/International Society of Oral Oncology (MASCC/ISOO) and the European Society for Blood and Marrow Transplantation (EBMT). Supportive Care in Cancer 23: 223–236.
Menezes, L., and J. R. Rao. 2012. Acute myelomonocytic leukemia presenting with gingival enlargement as the only clinical manifestation. J Indian Soc Periodontol 16: 597–601.
Sollecito, T. P., J. Draznin, E. Parisi, K. Duffy, E. A. Stadtmauer, S. M. Luger, S. J. Schuster, D. Tsai, and D. L. Porter. 2003. Leukemic gingival infiltrate as an indicator of chemotherapeutic failure following monoclonal antibody therapy: a case report. Spec Care Dentist 23: 108–110.
Chen, L., H. M. Linden, B. O. Anderson, and C. I. Li. 2014. Trends in 5-year survival rates among breast cancer patients by hormone receptor status and stage. Breast Cancer Res Treatment 147: 609–616.
Rizvanov, A. A., M. E. Yalvac, A. K. Shafigullina, Salafutdinov, II, N. L. Blatt, F. Sahin, A. P. Kiyasov, and A. Palotas. 2010. Interaction and self-organization of human mesenchymal stem cells and neuro-blastoma SH-SY5Y cells under co-culture conditions: A novel system for modeling cancer cell micro-environment. Eur J Pharm Biopharm 76: 253–259.
Dogan, A., S. Demirci, H. Apdik, E. A. Apdik, and F. Sahin. 2017. Dental pulp stem cells (DPSCs) increase prostate cancer cell proliferation and migration under in vitro conditions. Tissue Cell 49: 711–718.
Raj, A. T., S. Kheur, R. Bhonde, V. R. Mani, H. A. Baeshen, and S. Patil. 2021. Assessing the effect of human dental pulp mesenchymal stem cell secretome on human oral, breast, and melanoma cancer cell lines. Saudi J Biol Sci 28: 6556–6567.
Shi, S., and S. Gronthos. 2003. Perivascular niche of postnatal mesenchymal stem cells in human bone marrow and dental pulp. J Bone Mineral Res 18: 696–704.
Izadirad, M., Z. Huang, F. Jafari, A. A. Hamidieh, A. Gharehbaghian, Y.-D. Li, L. Jafari, and Z.-S. Chen. 2021. Extracellular vesicles in acute leukemia: A mesmerizing journey with a focus on transferred microRNAs. Frontiers Cell Dev Biol 9: 766371.
Savanur, V. H., A. Sarkar, A. Petryna, K. Nguyen, J. Benites-Sandoval, M. Gergues, A. Hatefi, and P. Rameshwar. 2024. A Platform to Establish a Working Hierarchy of Glioblastoma Multiforme Cells:: Implication on Cancer Cell-microenvironment Interaction and Response to Drugs. Intl J Transl Sci: 177–200.
Tsolaki, I., D. Rojas, A. Eljarrah, and P. Rameshwar. 2024. Isolating Dental Pulp Stem Cells. In Stepwise Culture of Human Adult Stem Cells. River Publishers. 45–52.
Patel, J. P., M. Gönen, M. E. Figueroa, H. Fernandez, Z. Sun, J. Racevskis, P. Van Vlierberghe, I. Dolgalev, S. Thomas, O. Aminova, K. Huberman, J. Cheng, A. Viale, N. D. Socci, A. Heguy, A. Cherry, G. Vance, R. R. Higgins, R. P. Ketterling, R. E. Gallagher, M. Litzow, M. R. van den Brink, H. M. Lazarus, J. M. Rowe, S. Luger, A. Ferrando, E. Paietta, M. S. Tallman, A. Melnick, O. Abdel-Wahab, and R. L. Levine. 2012. Prognostic relevance of integrated genetic profiling in acute myeloid leukemia. N Engl J Med 366: 1079–1089.
Tallman, M. S., E. S. Wang, J. K. Altman, F. R. Appelbaum, V. R. Bhatt, D. Bixby, S. E. Coutre, M. De Lima, A. T. Fathi, M. Fiorella, J. M. Foran, A. C. Hall, M. Jacoby, J. Lancet, T. W. LeBlanc, G. Mannis, G. Marcucci, M. G. Martin, A. Mims, M. R. O’Donnell, R. Olin, D. Peker, A. Perl, D. A. Pollyea, K. Pratz, T. Prebet, F. Ravandi, P. J. Shami, R. M. Stone, S. A. Strickland, M. Wieduwilt, K. M. Gregory, L. Hammond, and N. Ogba. 2019. Acute Myeloid Leukemia, Version 3.2019, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Net 17: 721–749.
Arber, D. A., A. Orazi, R. Hasserjian, J. Thiele, M. J. Borowitz, M. M. Le Beau, C. D. Bloomfield, M. Cazzola, and J. W. Vardiman. 2016. The 2016 revision to the World Health Organization classification of myeloid neoplasms and acute leukemia. Blood 127: 2391–2405.
Moore, C. A., Z. Siddiqui, G. J. Carney, Y. Naaldijk, K. Guiro, A. I. Ferrer, L. S. Sherman, M. Guvendiren, V. A. Kumar, and P. Rameshwar. 2021. A 3D Bioprinted Material That Recapitulates the Perivascular Bone Marrow Structure for Sustained Hematopoietic and Cancer Models. Polymers (Basel) 13.
Castillo, M., K. Liu, L. Bonilla, and P. Rameshwar. 2007. The immune properties of mesenchymal stem cells. Int J Biomed Sci 3: 76–80.
Sinha, G., A. I. Ferrer, S. Ayer, M. H. El-Far, S. H. Pamarthi, Y. Naaldijk, P. Barak, O. A. Sandiford, B. M. Bibber, G. Yehia, S. J. Greco, J. G. Jiang, M. Bryan, R. Kumar, N. M. Ponzio, J. P. Etchegaray, and P. Rameshwar. 2021. Specific N-cadherin-dependent pathways drive human breast cancer dormancy in bone marrow. Life Sci Alliance 4:e202000969.
Patel, S. A., S. H. Ramkissoon, M. Bryan, L. F. Pliner, G. Dontu, P. S. Patel, S. Amiri, S. R. Pine, and P. Rameshwar. 2012. Delineation of breast cancer cell hierarchy identifies the subset responsible for dormancy. Sci Rep 2: 906.
Dubois, F., M. Bénard, B. Jean-Jacques, D. Schapman, H. Roberge, A. Lebon, D. Goux, B. Monterroso, N. Elie, and H. Komuro. 2020. Investigating tunneling nanotubes in cancer cells: Guidelines for structural and functional studies through cell imaging. BioMed Res Intl 2020: 2701345.
Patel, S. A., M. A. Dave, S. A. Bliss, A. B. Giec-Ujda, M. Bryan, L. F. Pliner, and P. Rameshwar. 2014. Treg/Th17 polarization by distinct subsets of breast cancer cells is dictated by the interaction with mesenchymal stem cells. J Canccr Stem Cell Res 2014.
Guerra, F., A. A. Arbini, and L. Moro. 2017. Mitochondria and cancer chemoresistance. Biochimica et Biophysica Acta (BBA)-Bioenergetics 1858: 686–699.
Greco, S. J., S. Ayer, K. Guiro, G. Sinha, R. J. Donnelly, M. H. El-Far, L. S. Sherman, Y. Kenfack, S. H. Pamarthi, M. Gergues, O. A. Sandiford, M. J. Schonning, J. P. Etchegaray, and P. Rameshwar. 2021. Restoration of aged hematopoietic cells by their young counterparts through instructive microvesicles release. Aging (Albany NY) 13: 23981–24016.
DiNardo, C. D., and A. H. Wei. 2020. How I treat acute myeloid leukemia in the era of new drugs. Blood 135: 85–96.
Tang, B., A. Raviv, D. Esposito, K. C. Flanders, C. Daniel, B. T. Nghiem, S. Garfield, L. Lim, P. Mannan, A. I. Robles, W. I. Smith, Jr., J. Zimmerberg, R. Ravin, and L. M. Wakefield. 2015. A flexible reporter system for direct observation and isolation of cancer stem cells. Stem Cell Reports 4: 155–169.
Tang, B., A. Raviv, D. Esposito, K. C. Flanders, C. Daniel, B. T. Nghiem, S. Garfield, L. Lim, P. Mannan, and A. I. Robles. 2015. A flexible reporter system for direct observation and isolation of cancer stem cells. Stem Cell Reports 4: 155–169.
Massberg, S., P. Schaerli, I. Knezevic-Maramica, M. Köllnberger, N. Tubo, E. A. Moseman, I. V. Huff, T. Junt, A. J. Wagers, I. B. Mazo, and U. H. von Andrian. 2007. Immunosurveillance by hematopoietic progenitor cells trafficking through blood, lymph, and peripheral tissues. Cell 131: 994–1008.
Bergmann, O. J., H. P. Philipsen, and J. Ellegaard. 1988. Isolated gingival relapse in acute myeloid leukaemia. Eur J Haematol 40: 473–476.